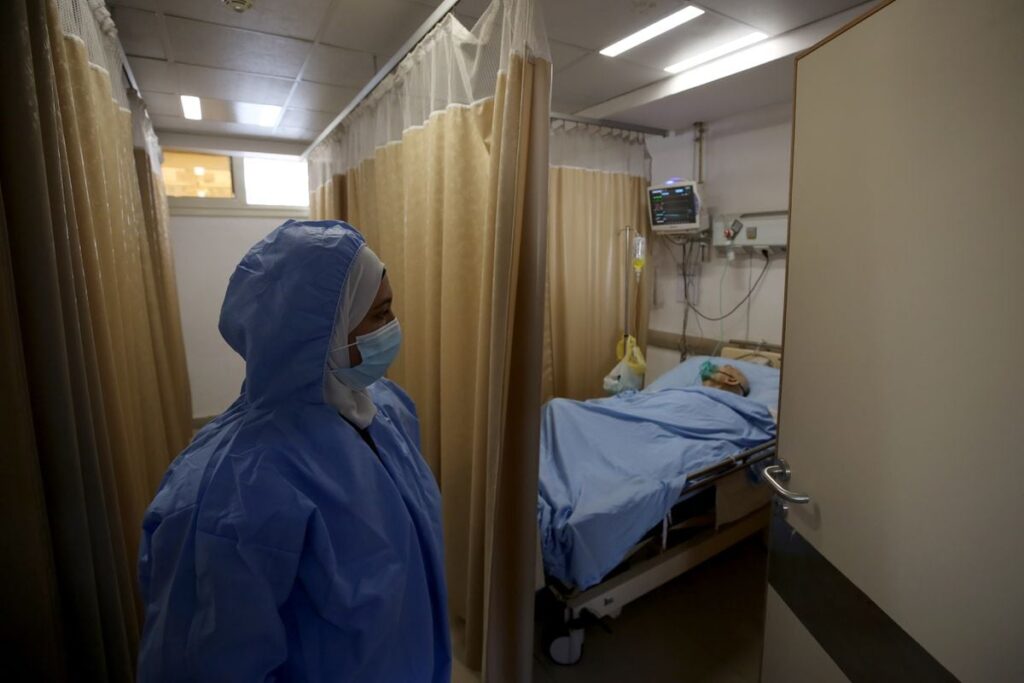
In early October, the World Health Organization (WHO) made an announcement that Cairo could only dream of a few years ago. He confirmed that Egypt, after an unprecedented national campaign against hepatitis C, has become the first country in the world which is on track to end the epidemic by 2030.
The achievement is all the more remarkable given the fact that, just a decade ago, Egypt was the country with the highest rates of hepatitis C in the world. But between 2014 and 2020, it launched one of its biggest health campaigns ever, aiming to wipe the disease off the map. It mobilized tens of thousands of its healthcare workforce, screened 50 million people and treated more than 4 million. Now, with success, lessons learned and recognition from the global health community assured, Cairo has decided to take it a step further and is helping other low- and middle-income countries, especially in Africa, to replicate its program.
“Egypt’s journey from having one of the highest rates of hepatitis C infection in the world to being on the road to elimination in less than 10 years is nothing short of amazing.” said WHO director-general Tedros Adhanom Ghebreyesus in October. “Egypt is an example in the world of what can be achieved with modern tools and political commitment at the highest level to use these tools to prevent infections and save lives,” he added. “Egypt’s success should give us all hope and motivation to eradicate hepatitis C everywhere.”
A polluted country
The origins of Egypt’s hepatitis C epidemic lie in a health campaign designed to treat an earlier epidemic. Between the 1940s and 1970s, the country had to deal, especially in rural areas, with a disease caused by contact with parasitic worms that lived in the polluted waters of the Nile, says Imam Waked, a professor from the department of hepatology at the National of Egypt . Liver Institute.
“Every family in Egypt has one [on average] at least one member infected with hepatitis C’.
Mohamed El-Kassas, professor and head of endemic medicine at Helwan University in Cairo
The only treatment available at the time for the disease was intravenous injections. But Waked says hepatitis was still unknown and disposable syringes were not available. So when the government began promoting a national campaign to combat the disease, starting in the 1950s, it inadvertently released the hepatitis C virus. To treat groups of between 500 and 600 young people, who were the main victims of the disease- target, 15 to 20 syringes could be used, the expert explains. “This is the age group that spread hepatitis C. We created a large population that had the virus, which then spread even more through blood transfusions, through health clinics and through more injections,” says the professor.
By the early 2000s, Nile disease had been virtually eradicated. However, in 2008, a demographic and public health survey found that 15% of Egyptians had hepatitis C antibodies, indicating that they had been exposed to the virus, and that 10% of people between the ages of 15 and 59 were living with chronic infection. Seven years later, in 2015, another study identified its presence in 7% of adults. But that decline was because hepatitis C was more common among older age groups — who had been treated for schistosomiasis decades earlier — than among young people, a factor that reduced the proportion of people who got hepatitis C, but that they don’t show that the total number of cases had decreased.
“For many years Egypt was labeled as the country with the highest rates of hepatitis C in the world,” says Mohamed El-Kassas, professor and head of endemic medicine at Helwan University in Cairo. “Every family in Egypt has one [on average] at least one member infected with hepatitis C,” he continues.
The consequences for the country have been equally dire: in 2015, hepatitis C caused the loss of approximately 40,000 lives, amounting to 7.6% of the country’s total deaths and responsible for reducing life expectancy by approximately 1.8 years for men and one year for women. It also caused the national GDP to decrease by 1.5% per year, or about $5 billion per year, according to World Bank estimates.
Faced with this challenge, Egypt established a national hepatitis C control committee in 2006 and two years later launched its first national campaign to expand access to treatment. The obstacles, however, were significant. Treatment for hepatitis C was very expensive, had serious side effects, few people were ultimately cured, and treatment could not be offered to people with advanced liver disease. “It wasn’t very good treatment. We treated 50,000 patients a year and we cured 15,000 to 20,000,” Waked recalls. “It was a huge burden on our health and our economy.”
Mobilized nation
The turning point came in late 2013, when hepatitis C treatment was revolutionized by a new oral antiviral drug that, when combined with other antivirals, increased the cure rate to more than 90% and almost completely eliminated side effects. The $84,000 price per treatment set by Gilead, the pharmaceutical company that patented the drug, became the main obstacle. But Egypt forced the company to negotiate that price after rejecting Gilead’s property license. Negotiations brought the price down to $900 per case, and then by licensing the drug to local pharmaceutical companies, Egypt lowered the cost to less than $84. This resulted in a 99.9% price drop, according to a 2021 study.
With the new drug, everyone who had previously been treated but not cured started the process over. By 2017, nearly all Egyptians known to be living with hepatitis C (about 2.3 million people) had received treatment, Waked says. However, health authorities knew that there were between 2 and 3 million people living with the disease who had not yet been diagnosed. It was at this point that, in late 2018, Cairo shifted to a much more ambitious strategy, shifting its focus from hepatitis C control to eradicating the disease. The 100 Million Healthy Lives campaign aimed to test more than 60 million people and offer free treatment to those living with the virus. Most of its funding came from government coffers, supplemented by a loan of about $250 million from the World Bank.
One of the most important aspects of the campaign was its speed. The state opened nearly 16,000 testing sites across the country, including 1,000 portable units that were accessible to walk-ins. Results were usually available within 20 minutes, and those found positive were sent to another site for confirmatory testing. Within seven days, those confirmed positive were taken to a center for treatment, which lasted 12 weeks, after which they were called back to a testing site to have their status checked.
Another of the main factors behind the success of the campaign was the strong political will to tackle the epidemic, including that of the country’s president, Abdel Fattah el-Sisi. The government has also launched a massive promotion and awareness campaign through media platforms, social networks, text messages and at the grassroots level. And it was just as important that it could tap into the country’s existing, neglected but extensive healthcare infrastructure. “It’s become a national priority for everyone: government, civil society, industry,” says John Ward, director of the Global Hepatitis Eradication Coalition. “There was a real commitment to health equity: all Egyptians had to benefit from the program.”
By the end of the campaign, about 50 million Egyptians had been tested. Of these, 2.2 million tested positive and took a confirmatory test, which verified the positive status of 1.6 million. In total, 900,000 cases were treated and another 700,000 more after the campaign ended. The recovery rate was 98%. The campaign was then extended to minors as well. Between May 2019 and January 2020, 3.8 million students were tested, according to former health service spokesman Khaled Megahed.
“Thanks to the campaign the percentage [of hepatitis C] it has gone from 10% to 0.3% or 0.4%. This is an incredible achievement,” says Ward. “It is one of the greatest achievements in global public health, at least in this century,” he adds.
And now, Africa
The success of Egypt’s campaign, and the experience gained along the way, have become important assets that WHO believes can be used by other low- and middle-income countries to develop their own plans to eliminate hepatitis C. Globally , about 75% of people living with the disease are in these two categories of countries, according to the health organization.
In Africa, the situation is significantly different from Egypt in its most difficult times, because hepatitis C is much less prevalent. Even in the countries struggling hardest with the virus, such as the Democratic Republic of Congo and Nigeria, the rates range from 3% to 4%, according to Waked.
Due in part to achieving the goal, Egypt’s then-health minister Hala Zayed announced at an African hepatitis summit in 2019 that Cairo, which at the time was chair of the African Union (AU), was ready to offer in all countries the rest of the continent technical support, expertise and free treatment for hepatitis C. It set an initial target of reaching 1 million people. “When we discovered that hepatitis C was easy to treat and that the medicine in Egypt was very cheap, we decided to help African countries in need of treatment by providing technical know-how, technology, advice and free medicine,” says Waked.
“It is very commendable that Egypt is extending health diplomacy to these countries,” says Ward. One of the first nations to benefit was Ghana, where a 2021 survey found that the rate of hepatitis C in a sample of 100,000 people was 2.6%, with significantly higher rates in its northern regions.
In March 2023, Egypt sent to Ghana the first donation of drugs to treat the disease, with the initial aim of making it available to people who have been diagnosed, but who cannot access treatment due to cost. Currently, patients still have to pay for their own tests to determine their viral load, which cost between $37 and $80. “A cheaper price or alternative tests would improve our ability tremendously,” says Waked.
Speaking on the same point, Ward points out that it’s not enough to just give out free drugs. “You have to get the other parts of it [Egypt’s] program for the use of these drugs. And that’s where technical assistance comes in, choosing the right partners in each country and then giving them the free drugs,” he says.
In addition to Ghana, Egypt’s health minister says that by early 2020, just over 30,500 citizens in South Sudan, Chad and Eritrea had been tested for hepatitis C and that about 400 had received free treatment. Waked says Egyptian health authorities are also in contact with The Gambia. And Ward believes Kenya, Tanzania, Uganda, Sierra Leone, Zambia and, to some extent, South Africa, could benefit from similar assistance.
Sign up for our weekly newsletter to get more English language news coverage from EL PAÍS USA