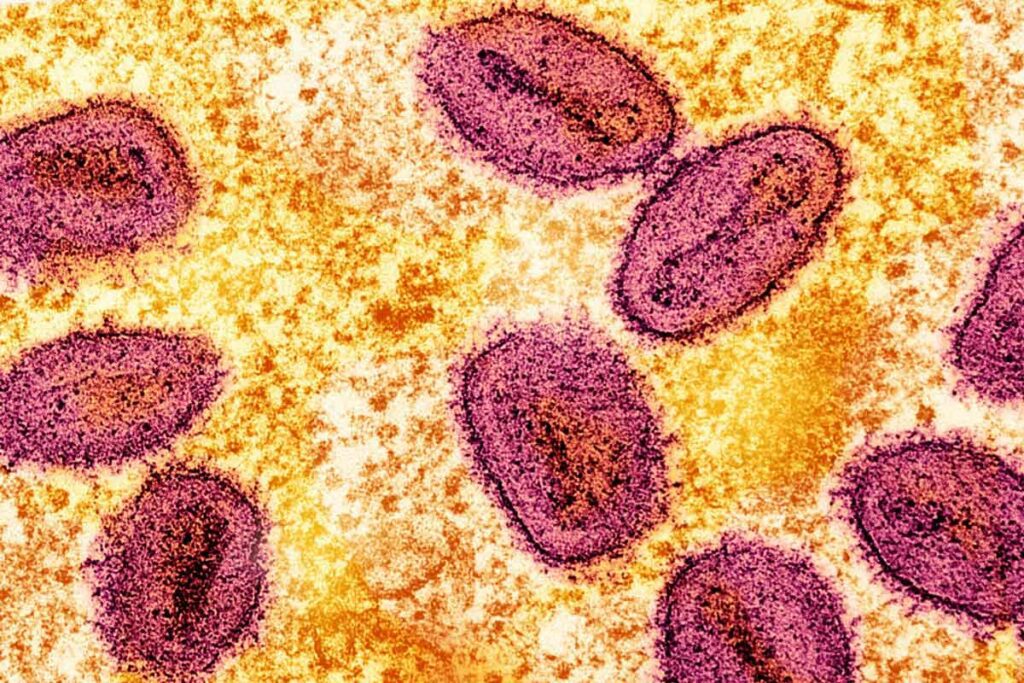
Until 2017, Professor Dimie Ogoina’s experiences with mpox were strictly theoretical. But all that would change in September of that year when he encountered the first clinical case of the disease in an 11-year-old boy at the Nigerian University Delta Teaching Hospital (NDUTH) in Bayelsa, Nigeria.
It was the first confirmed case of the disease in Nigeria since 1978, but also the beginning of an unfolding epidemic. With DecemberOgoina had managed a significant proportion of the more than 200 cases reported across the country that year – and the majority of his patients were young, male adults between the ages of 20 and 40.
Although alarming, the observation that mpox could infect young adults piqued Ogoina’s curiosity, especially since the disease had historically been reported in young children. But that wasn’t all he discovered.
“What was also remarkable was that the majority of these people [the young male adults] who presented with mpox had unusual lesions or skin rashes around the genital area, with ulcers. That seemed very unusual,” he says.
This unusual find drove his curiosity further, setting him on a long learning curve that would lead to both new discoveries and the constant scrutiny of the scientific community. It also laid the groundwork for his proposal that mpox could be transmitted through sexual contact.
While Ogoina’s work was largely based on the Clade II virus common in West Africa, his findings have continued to inform responses to mpox outbreaks around the world.
In 2023, Ogoina was listed as one of the Hour 100 Most Influential People, in recognition of his work on mpox, which by that time had garnered much global attention.
Challenges hinder efforts to tackle mpox
Mpox is a zoonotic disease, capable of being transmitted both from animal to human and from human to human. Although various animal reservoirs, including squirrels, rats, and monkeys, may contribute to the transmission of the disease in human populations, the exact cycle of transmission remains an unresolved puzzle.
Since the first case appeared in 1970, numerous cases of mpox have been reported in the Democratic Republic of the Congo (DRC), mainly caused by the Clade I strain of the virus. Unlike the Clade II mpox virus, which caused the 2022 global outbreak, the Clade I strain presents with more severe symptoms, with a mortality rate of up to 10%.
In a recent correspondence article published in Nature Medicine, the authors wrote that mpox “is emblematic of the global neglect of diseases endemic to Africa until they threaten the health security of the Global North. Progress must be made to control this disease and gaps must be addressed to achieve global health security.” They highlighted gaps in laboratory testing and timely access to diagnostics, treatments and vaccines as key factors driving the spread of mpox in the DRC and by extension, Africa.
In an interview with VaccinesWork, Dr Daniel Mukadi-Bamuleka, who researches mpox and other emerging diseases such as Ebola in the DRC, added negligence, low interest and limited funding to this list.
The need for more investment is still huge
Between 11 and 13 April, a “High-Level Regional Emergency Meeting on Mpox in Africa” was held in Kinshasa, DRC. The event provided a platform to discuss the epidemiology of mpox, strengthen collaborations between key stakeholders and partners such as CEPI, WHO and UNICEF, and develop a robust action plan to address the disease on the continent. During this meeting, WHO and its partners committed to providing diagnostic and treatment packages to care facilities in remote areas to ensure a more decentralized and timely response to the ongoing outbreak.
Reflecting on the progress made during the meeting, Dr Beatrice Umba di Nguete, Technical Coordinator at the CDC/Kinshasa School of Public Health (KSPH), says: “The need is still huge, but efforts are ongoing.” Dr Placide Mbala-Kingebeni, who was also present at the meeting, says joint teams from the Ministry of Health have been deployed to conduct active disease surveillance, including investigation of sexually transmitted cases, in the affected areas. Mbala-Kingebeni, an associate professor at the University of Kinshasa School of Medicine, heads the Department of Epidemiology and Global Health at the INRB (Institut National de la Recherche Biomédicale), DRC. While these interventions have the potential to pave the way for progress, he adds that limited funding still hampers the efforts of scientists on the ground.
Sexual transmission
WHO first issued an alert on sexual transmission and emergence of Clade I mpox in new provinces of the DRC on November 3, 2023. While sexual transmission of mpox may no longer surprise scientists, it once did: before 2017, when Ogoina began noticing a new type of mpox in the patients he managed at his university teaching hospital. These patients not only differed in their demographics, being young male adults, but they also presented with symptoms unusual for classic mpox. Instead of a generalized rash, they developed genital rashes and ulcers and often contracted sexually transmitted infections, such as HIV or syphilis.
When Ogoina suggested that this new, sexually transmissible mpox was free, the scientific community questioned the truth of his claims. But he was convinced of the case he made from these observations, describing them as “too remarkable to be ignored”. On July 23, 2022, the WHO stated mpox Public Health Emergency of International Concern (PHEIC) after it started appearing in new areas around the world. Similar to Ogoina’s earlier observations, the cases were largely reported in men, and most of these men identified as gay and bisexual.
Vaccines, diagnostics and therapeutics to control outbreaks
While the world has recovered from the mpox outbreak of 2022, the DPRK continues to struggle with the burden of a disease that never seems to go away. As of May 26, 7,851 cases and 384 deaths had been recorded mentionted of mpox in 177 of the 519 health zones and 22 of the 26 provinces of the PRC. More recently data from Africa The CDC says 97% of the 8,479 cases reported in seven African countries so far, as of June 14, are from the DRC.


In addition to the increasing number of cases of the disease, Mbala-Kingebeni, who has been researching mpox since 2008, says significant progress has been made in recent times. “There are more cases being detected because we now have the ability to diagnose directly in the field. We have Gene Xpert and cartridges, so we are able to quickly diagnose and provide supportive care.” He adds that an ongoing clinical trial, led by INRB and NIH, is testing the efficacy and safety of tecovirimat, an antiviral drug originally developed for smallpox, against mpox.Findings are expected to be available later this year.
Results from a more comprehensive mpox vaccine trial in healthcare workers are also promising. However, there is a need for an efficacy study to validate them. He expects the study could be conducted by 2025.
The road ahead
Despite these many interventions, the disease is unlikely to be eradicated anytime soon. The absence of serological tests, therapeutics and vaccines, combined with poor health-seeking behaviours, weak surveillance systems and obscure animal pools complicate the ongoing battle. While increased investment in mpox research and development could address these issues, Ogoina also strongly advocates improving awareness of the sexually transmitted new mpox – of course without neglecting the classic mpox.
Eradication or elimination of mpox may not be in sight, but vaccines remain the key to breaking the chain of transmission, fighting infection and preventing disease in endemic areas, argues Mbala-Kingebeni.